
Spring Skincare Swap: Which Winter Products to Ditch (and What to Use Instead)
Table of Contents Introduction After months of relying on rich moisturizers, thick balms, and barrier-repair creams, spring is the season when many of those winter
Shannon Del Grande is now seeing patients in our Wayne/Chesterbrook office.
One of the most common skin concerns is facial redness, and it is also one of the most misunderstood. Occasional flushing is mostly harmless, but persistent redness may indicate a chronic condition like rosacea, which affects an estimated 5% of the global population and often goes undiagnosed.
Rosacea is an inflammatory skin condition that occurs and develops over long periods of time. It typically affects the central face, especially the cheeks, nose, forehead, and chin. It can appear as flushing, visible blood vessels, or acne-like bumps, and symptoms often come and go in cycles.
Redness can be caused by many factors including environmental triggers and skin sensitivity. It’s not always easy to tell whether what you’re experiencing is temporary irritation or something more persistent like rosacea.
In this article, we’ll break down how to tell the difference between normal skin redness and rosacea, review the key signs to look for, and explain when it’s time to seek professional evaluation. For a deeper clinical overview of rosacea, you can explore this trusted resource from the National Institutes of Health (NIH) Rosacea Overview.
If you’re already noticing ongoing redness or sensitivity, you can also learn more about evaluation and treatment options at Bryn Mawr Dermatology, where personalized care can help clarify your diagnosis and guide next steps.
While this article spells out some important information about Rosacea, we highly recommend you read the full article, here are the key points we will focus on:

Rosacea is more than just occasional redness. It is a chronic inflammatory skin condition, that if left unmanaged it can affect both the appearance and sensitivity of the skin. Initially, it can go unnoticed, but over time, it can evolve into more persistent and noticeable symptoms.
Clinically, rosacea most commonly presents as facial flushing, persistent redness (erythema), visible blood vessels (telangiectasia), and in some cases, acne-like bumps. You can usually see the redness confined to the center of the face. It usually swings back and forth between flare-ups and remissions.
Epidemiologically, rosacea is estimated to affect over 415 million people worldwide, with higher prevalence among individuals aged 30–50 and those with fair skin. Studies have also shown that up to 40% of patients report a family history, suggesting a genetic component.
Additionally, research published through institutions like the National Institutes of Health highlights the role of immune system dysregulation and vascular sensitivity in its development.
Although rosacea is not dangerous, early recognition is important, timely diagnosis and treatment can significantly reduce symptom progression and improve skin health over the long term.
Rosacea typically begins with episodes of flushing that gradually become more constant over time. What may initially appear as mild redness after triggers like heat, stress, or certain foods can evolve into a more permanent background redness with visible blood vessels.
In some individuals, inflammatory bumps develop alongside redness, which can easily be confused with acne, but unlike acne, rosacea does not involve blackheads. The skin may also feel more reactive overall, with increased sensitivity to skincare products, weather changes, or environmental factors.
Rosacea flare-ups are often influenced by everyday factors that increase blood flow to the skin or trigger inflammation. Identifying these triggers is a key part of managing symptoms and reducing the frequency of flare-ups.
Research from the National Rosacea Society shows that sun exposure aggravates rosacea in 81% of patients and emotional stress in 79%, and many identify multiple factors that worsen their symptoms over time.
Triggers vary widely between individuals, which is why rosacea can feel unpredictable. What causes a flare in one person may not affect another at all. However, environmental factors, especially sun exposure and temperature changes, are consistently among the most reported contributors.
Over time, repeated exposure to triggers can make redness more persistent, as the skin’s blood vessels become increasingly reactive. Keeping a simple record of flare-ups and potential triggers can help identify patterns, making it easier to avoid or minimize exposures and better control symptoms.
While these conditions can overlap in appearance, rosacea tends to follow a distinct pattern—persistent central facial redness, visible blood vessels, and flare-ups triggered by specific environmental or lifestyle factors. Unlike acne, rosacea does not involve clogged pores, and unlike eczema, it typically does not cause intense itching.
Because symptoms can mimic one another, self-diagnosis isn’t always reliable. If redness is ongoing, worsening, or accompanied by sensitivity or bumps, a professional evaluation can help confirm whether it’s rosacea or another condition, and ensure you’re treating it effectively rather than unintentionally making it worse.
Rosacea isn’t a one-size-fits-all condition—it’s classified into subtypes based on how it appears and progresses. Understanding these distinctions can help clarify your symptoms and guide more targeted treatment.
Clinical research supported by organizations like the National Institutes of Health shows that many patients experience features of more than one subtype at the same time, which is why proper diagnosis is essential.
While these categories help define rosacea, many individuals experience overlapping symptoms, making self-identification challenging. Recognizing your specific pattern is important, not just for diagnosis, but for choosing treatments that effectively address your unique presentation.
While rosacea can’t be permanently cured, it can be effectively managed with the right combination of treatments and lifestyle adjustments. The goal is to reduce inflammation, control flare-ups, and improve overall skin appearance.
Clinical guidance from the American Academy of Dermatology shows that a tailored, multi-approach treatment plan significantly improves symptoms in most patients, particularly when started early and adjusted over time.
Because rosacea varies from person to person, treatment is rarely one-size-fits-all. A personalized plan developed with a dermatology provider ensures the most effective and sustainable results.
In many cases, people notice that their skin looks better for weeks or even months, leading them to believe the issue has been resolved. However, these periods of improvement are usually temporary. Over time, untreated rosacea can become more noticeable, with longer-lasting redness and increased skin sensitivity.
Persistent redness can be confusing, but as we’ve covered, rosacea has distinct patterns, triggers, and treatment pathways that require expert evaluation. Identifying the right diagnosis is the first step toward getting your skin back under control.
At Bryn Mawr Dermatology, care is personalized, evidence-based, and tailored to your specific skin type and rosacea subtype. Rather than a one-size-fits-all approach, their team develops customized treatment plans that may include prescription therapies, advanced laser options, and guidance on trigger management, all designed to deliver long-term results.
What sets Bryn Mawr Dermatology apart is their combination of clinical expertise and patient-centered care. From your initial consultation to ongoing follow-up, the focus is on precision, comfort, and outcomes, ensuring your treatment evolves as your skin improves.

Published By: Bryn Mawr Dermatology
Medically Reviewed By: Christine Stanko, MD, FAAD

Table of Contents Introduction After months of relying on rich moisturizers, thick balms, and barrier-repair creams, spring is the season when many of those winter
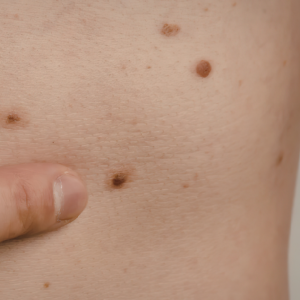
Don’t wait for summer to prioritize your skin health. Book your annual skin check today. Call us to schedule your appointment.

Discover how multifrax compares to traditional fractional lasers and why it delivers better precision and faster recovery.
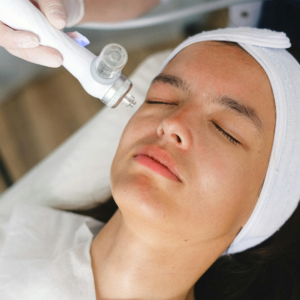
Winter is the ideal time for peels, lasers, and CO₂ treatments with less sun exposure, smoother recovery, and better skin results.

Learn how to prevent and treat winter skin flare-ups with expert tips on hydration, skincare routines, and in-office treatments.

Healthy Skin Month is here! Discover how to protect your skin this winter and book your skincare consultation today!

By: Bryn Mawr Dermatology, Published: June 25, 2024
Medically Reviewed By: Christine Stanko, MD, FAAD – June 25, 2024
For COSMETIC APPOINTMENTS:
For MEDICAL APPOINTMENTS: